What is TMD? How can I alleviate discomfort from TMJ?
Symptoms, Remedies, Treatment Options, and More
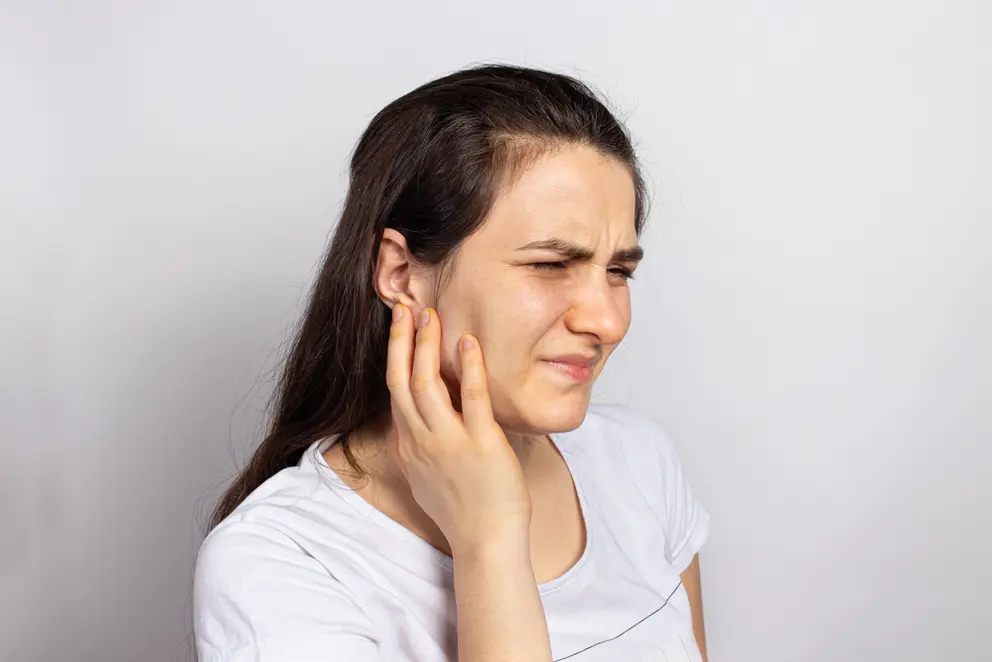
If you’re experiencing jaw discomfort like locking, popping, stiffness, or soreness, you might have a common condition called Temporomandibular Joint Disorders (TMD). According to the National Institute of Health, this disorder affects between 5-12% of Americans, twice as many women as it does men, and more younger patients than older ones, which is unusual for chronic pain conditions.
Explore your options with a consultation